What’s killing American females?
 Monday, February 11, 2013 at 06:31PM
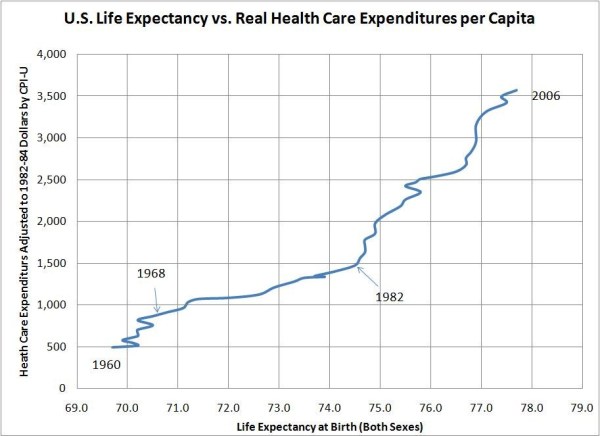
Monday, February 11, 2013 at 06:31PM This question emerged unexpectedly from my post on US healthcare efficiency did not go off the rails until about 30 years ago. Lane Kenworthy posted the following graph to show that, when compared to all of 19 other wealthy OECD nations, US per-capita health care expenditures went through the roof while simultaneously delivering much smaller gains in life expectancy at birth.

My initial reaction was that something happened to accelerate the rate of spending increases in America. It did not occur to me that there had been a divergence in life expectancy improvement. However, taking the data apart revealed just the opposite: The rate of increase in real US per-capita health care expenditures has been steadily shrinking since at least 1960 but, starting in about 1983, America diverged downward from the peer nations in the rate of life expectancy improvements.
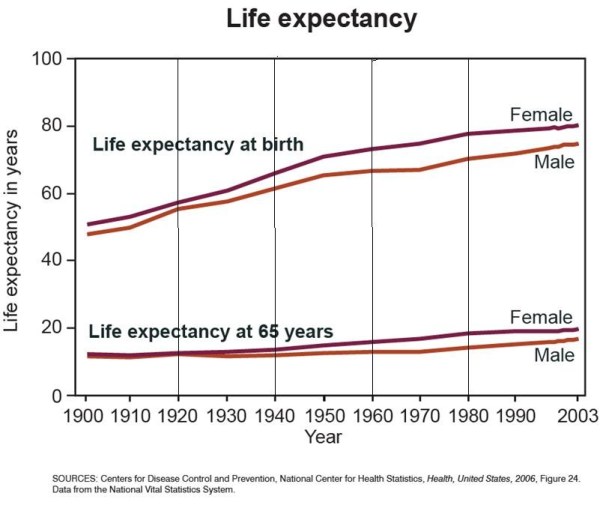
Digging a little deeper it appeared that most of the adverse divergence was attributable to females and that males continued to have life expectancy gains at about the same rate as in the recent past.
Why that happened was a complete mystery to me until the publication last month of U.S. Health in International Perspective: Shorter Lives, Poorer Health by the National Academy of Sciences. Hat tip Sabrina Tavernise at NYT. This is a monumental report of nearly 400 pages that is by no means focused on my question, "What's killing American females?" but there are clear partial explanations.
First, the study confirms that the US has been at or near the bottom in life expectancy and in the rate of increase in life expectancy and that the adverse divergence is almost entirely caused by US females.
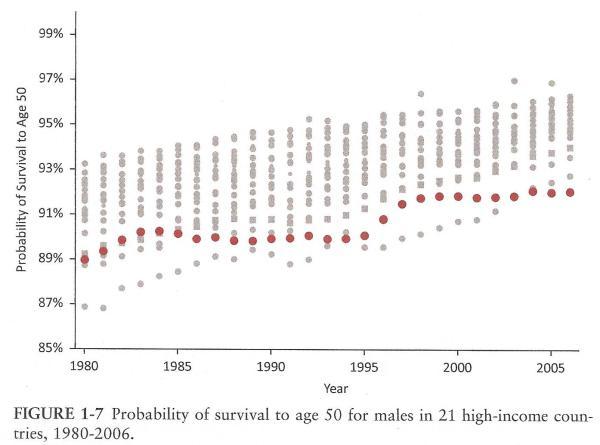
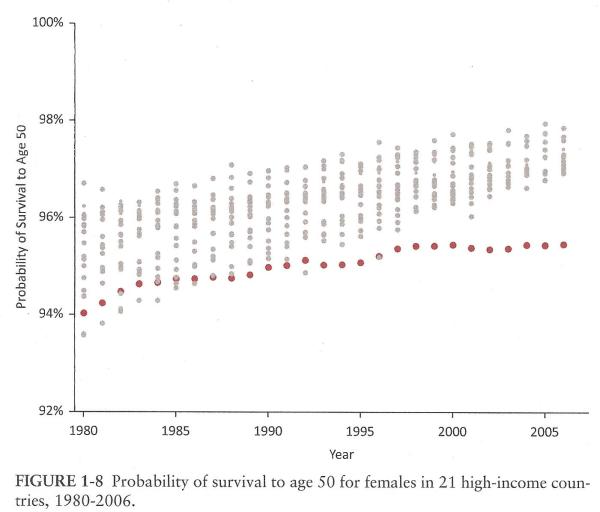
These charts show the probabilities of surviving to age 50, which the report tells us is the age range that primarily accounts for the US's life expectancy disadvantage. Indeed, after age 75, the life expectancy of Americans is higher than in peer nations. At 3.
One striking finding is that US death rates are higher than the mean of peer nations for almost all causes of death and is not near the best with respect to any cause of death. Table 1.2.
The report doesn't tell us what changed since 1983, but it does tell us which causes of death account for the poor showing of American females versus the mean of 16 peer nations in the 2006-08 time interval. Fully 37% of the excess deaths of American females occur from accidents and homicides, which are not normally thought of as "medical problems" that a better "health care system" might ameliorate.
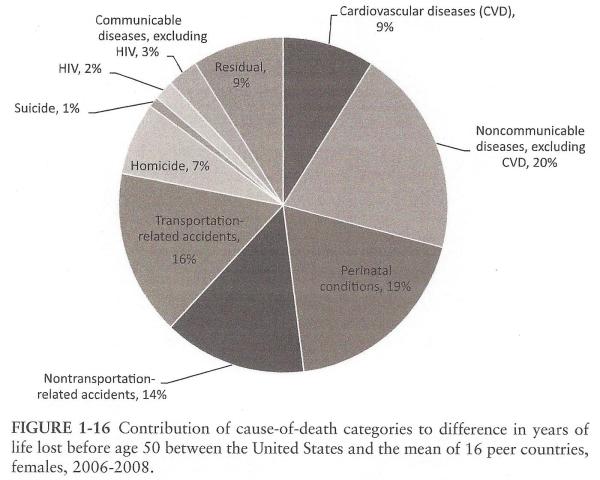
On the other hand, American females also lag their peers in deaths due to perinatal conditions, cardiovascular diseases, and other non-communicable diseases. Do American females have higher incidences of those maladies, or are they not getting as good treatment as in the peer nations? I don't think this report answers that.
Because the report provides only a snapshot from 2006-08, the report is unable to identify the causes of death most responsible for putting American females on their lower life expectancy trajectory in about 1983. Indeed, Recommendation 6 is to investigate how different policies may explain cross-national differences over time.
I'm sure this is not the most important health policy question of all time, but I found it intriguing and am glad to have partial answers. I'm even more pleased that the NAS and others are addressing in a thorough fashion what is making us sick and killing us and what policies have been found effective to improve our health.
None of this should distract us in any way from the disastrous growth since the early 1980s in per-capita health care spending that did not improve our lives. Well, I guess it improved the lives of health care vendors, but not my life. Or yours.
 Skeptic
Skeptic
I've continued to think about this and read some more of the report because the partial answer to the question I posed was not very satisfying. Perhaps it's not the best question to be asking because it appears we could learn a great deal about why US life expectancy gains slowed among females starting in about 1983 by examining differences among regions, states, and localities within the US. From Box 1-2 of the Report:
The range of life expectancies across U.S. states, which is 7.0 years for males and 6.7 years for females, exceeds the cross-national range between the United States and peer countries, which is 3.7 years for males and 5.2 years for females . . . . Although life expectancy is very low in Appalachia and the Deep South, some states in the northern Plains and along the Pacific coast and Eastern seaboard easily outrank many peer countries. . . .
Even greater disparities are found at the county level.
 Skeptic
Skeptic
The Associated Press reports on another study released today by the Journal of Health Affairs finding life expectancies for American females under 75 actually declining in some areas, while a much smaller effect was observed for men. The story reports speculations as to causes by the study authors and by other experts, but there is no consensus and no definitive evidence.
[ADDED 4/7/13] More detail in The Daily Mail and a graph on this study: Mortality rates for women are increasing in over 43% of U.S. counties compared to just 3.4% for men. There are strong regional patterns, and this article points the finger of causation more directly at socioeconomic factors than at lifestyle factors (without suggesting why women should be affected more than men):
According to the research, counties with higher population densities saw greater reductions in female mortality rates, as did counties with high average household incomes and a higher percentage of college graduates.
In areas where there was a high percentage of adult smokers there was an increased mortality rate.
Counties in the south and west had the highest increase in female mortality rates over the period.
'Many people believe that medical care and individual behaviors such as exercise, diet, and smoking are the primary reasons for declines in health,' the study said.
'We did find significant associations between mortality rates and some of these factors, such as smoking rates for both sexes. But socioeconomic factors such as the percentage of a county’s population with a college education and the rate of children living in poverty had equally strong or stronger relationships to fluctuations in mortality rates.'

 Skeptic
Skeptic
J. Paul Leigh at Economic Policy Institute says there is evidence that low wages alone contribute to morbidity and mortality in American females in several ways:
But it is not just obesity that may be affected by increasing the minimum wage. Juan Du and I use the PSID to consider wage and hypertension correlations. We analyze data on roughly 5600 adults from 1999 to 2005. We find that low wages in baseline years predict whether respondents will be newly diagnosed with hypertension in subsequent years. We find these predictions to be especially strong for women and persons under age 40, and these two groups are more likely than men over age 40 to be employed in low-wage jobs. This study was recently published in the European Journal of Public Health.
Finally, scores of studies in economics and epidemiology link low income to health problems including diabetes, heart disease, arthritis, and premature mortality.
The mechanisms through which low wages adversely affect health are varied, but two stand out. First, low wages can result in financial stress. Workers and their families may face persistent hassles associated with finding funds to pay for rent, electricity, groceries, and gas for the car. Even if the low-income family has insurance, funds for blood pressure and cholesterol medicines may not be available if the family must make co-payments and pay deductibles. The stress and lack of medicines likely adversely affect health. Second, many people partially assess their self-worth based on their wage. Unrelenting, long-term feelings of low self-worth likely also have negative consequences for health.
Well, it's all plausible but not in my opinion proven that raising the minimum wage or otherwise aleviating poverty is a good way to get life expectancies for American females to start improving again at the pre-1980 rate. For one thing, it isn't established that obesity, hypertension, and other health conditions don't cause people to gravitate to the bottom of the income scale instead of being caused by low income. Clearly all of these statistical measures are associated, but which causes what, and what's the best place to break into what is potentially a complex set of interactions?
 Skeptic
Skeptic
In the previous update, I said it wasn't clear which way the arrow of causation flies--does poverty cause high morbidity and mortality, or does poor health cause poverty? However, a randomized controlled study in Florida in the 1990s showed convincingly that welfare recipients in the arm with reduced welfare payments had shorter life expectancies than those in the arm with the more generous welfare scheme. Robert Waldman has a story on that at Angry Bear.
From 1994 to 1999, Florida randomly selected a group of welfare recipients into either the Family Transition Program (FTP), a program that included many features of the later PRWORA, or the then-standard Aid for Families with Dependent Children welfare program (AFDC). Muennig and his colleagues looked at Social Security Records for 3,224 participants in the experiment to establish whether participants had died in the 18 years following the randomization.
What they found was that participants in the experimental group had a 16 percent higher mortality rate than members of the control group (hazard ratio: 1.16; 95% confidence interval: 1.14, 1.19; p < 0.01). This amounts to nine months of life expectancy lost between the ages of thirty and seventy for people in FTP.”This was a surprise: Muennig et al. had expected that the increased employment associated with FTP would lead to improved health. Instead, FTP harmed the participants.
 Skeptic
Skeptic
NYT today has a front page article on a recent publication by Nobel laureate Angus Deaton and his wife Anne Case showing the increase in mortality among middle-aged Americans is largely due to suicide and drug and alcohol poisoning in white Americans with only a high school education or less. This is the abstract of the publication:
This paper documents a marked increase in the all-cause mortality of middle-aged white non-Hispanic men and women in the United States between 1999 and 2013. This change reversed decades of progress in mortality and was unique to the United States; no other rich country saw a similar turnaround. The midlife mortality reversal was confined to white non-Hispanics; black non-Hispanics and Hispanics at midlife, and those aged 65 and above in every racial and ethnic group, continued to see mortality rates fall. This increase for whites was largely accounted for by increasing death rates from drug and alcohol poisonings, suicide, and chronic liver diseases and cirrhosis. Although all education groups saw increases in mortality from suicide and poisonings, and an overall increase in external cause mortality, those with less education saw the most marked increases. Rising midlife mortality rates of white non-Hispanics were paralleled by increases in midlife morbidity. Self-reported declines in health, mental health, and ability to conduct activities of daily living, and increases in chronic pain and inability to work, as well as clinically measured deteriorations in liver function, all point to growing distress in this population. We comment on potential economic causes and consequences of this deterioration.
An earlier NYT article focused on increasing mortality among white non-Hispanic women but not specifically on an age group or particular causes of death.
The steepest declines were for white women without a high school diploma, who lost five years of life between 1990 and 2008, said S. Jay Olshansky, a public health professor at the University of Illinois at Chicago and the lead investigator on the study, published last month in Health Affairs. By 2008, life expectancy for black women without a high school diploma had surpassed that of white women of the same education level, the study found.
White men lacking a high school diploma lost three years of life. Life expectancy for both blacks and Hispanics of the same education level rose, the data showed. But blacks over all do not live as long as whites, while Hispanics live longer than both whites and blacks.
One comment in this article suggests that the correlation may not be with education per se but with declining economic circumstances, which may occur despite adequate education and may not be ameliorated in the short-term (or ever) by more education:
The five-year decline for white women rivals the catastrophic seven-year drop for Russian men in the years after the collapse of the Soviet Union, said Michael Marmot, director of the Institute of Health Equity in London.


Reader Comments (3)
When you visit rural Ohio, you see "tons" of overweight girls and women. You might see fewer beefy men because more of them are working outdoors in construction, heavy farm work, etc. I get the impression that more men than women go hunting.
If you ever read The China Study, you would have learned that our diet is worse for us than smoking is. The volumes of meat and dairy we eat are harmful. I believe meat should be used sparingly.
I've posted an update today with information about one study that seems to show clearly that poverty causes poor health.
I had not heard of The China Study referred to by Sandy. Wikipedia has a summary here: http://en.wikipedia.org/wiki/The_China_Study_(book) Very compelling.